
Suffering Foot or Ankle Pain or Discomfort?
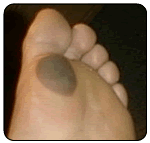 Blisters form as a result of heat, moisture and friction. Blisters can also form as a result of fungal infections of the skin, allergic reactions or burns. If a patient has diabetes, they should be evaluated by a doctor in a timely fashion. Generally, a person will recognize a burn by association with a specific painful event. People with diabetes may not be able recognize the painful event due to a condition called neuropathy. A doctor should attend to burns. Blisters are due to fungal infection of the skin or to allergic reactions, which will generally occur in clusters and be smaller than blisters caused by friction. They will also often occur in areas of the foot, which are free from friction forces.
Blisters form as a result of heat, moisture and friction. Blisters can also form as a result of fungal infections of the skin, allergic reactions or burns. If a patient has diabetes, they should be evaluated by a doctor in a timely fashion. Generally, a person will recognize a burn by association with a specific painful event. People with diabetes may not be able recognize the painful event due to a condition called neuropathy. A doctor should attend to burns. Blisters are due to fungal infection of the skin or to allergic reactions, which will generally occur in clusters and be smaller than blisters caused by friction. They will also often occur in areas of the foot, which are free from friction forces.
 Blisters should be drained leaving the cover of the blister intact. The area should be protected with a non-stick bandage with mild compression. Ice to "hot spots" can be soothing and reduce the thermal damage to the surrounding area. "Double socking" can prevent blisters associated with athletics. Wearing two pair of socks allows the friction to be absorbed between the socks, reducing friction to the skin. A sock has been developed that helps to reduce friction and blistering called the Thro-lo sock. It is useful for athletics and for diabetic patients. They are widely available in athletic shoe and apparel stores. Skin protectant sprays and adhesive gel pads are also available.
Blisters should be drained leaving the cover of the blister intact. The area should be protected with a non-stick bandage with mild compression. Ice to "hot spots" can be soothing and reduce the thermal damage to the surrounding area. "Double socking" can prevent blisters associated with athletics. Wearing two pair of socks allows the friction to be absorbed between the socks, reducing friction to the skin. A sock has been developed that helps to reduce friction and blistering called the Thro-lo sock. It is useful for athletics and for diabetic patients. They are widely available in athletic shoe and apparel stores. Skin protectant sprays and adhesive gel pads are also available.
Abrasions to the skin are a result of excessive friction resulting in the partial loss of the epidermis. The area should be cleaned with an antibacterial soap and dressed with a non-stick bandage and a topical antibiotic ointment. It may take several weeks for the area to completely heal. During this period, the area should be protected from shearing forces. Deep abrasions can result in scarring. Any sign of infection should prompt a visit to the doctor.
Skin Tears
Skin tears result from a rapid, forceful shear to the skin. Skin tears are most commonly self-inflicted by improperly removing adhesive dressings and tape. Careful counter pressure should be applied to the skin near the adhesive dressing as the dressing or tape is slowly removed. A common misconception is that paper tape will not damage the skin. To the contrary, this tape can really stick to the skin and will tear the skin if removed improperly.
